|
Dr Tom Cromarty Editor Interests: Paediatric Emergency Medicine, Medical Engagement and Leadership, Simulation, Quality Improvement, Research Twitter: @Tomcromarty |
Welsh Research and Education Network
WREN BlogHot topics in research and medical education, in Wales and beyond
Dr Celyn Kenny Editor Interests: Neonates, Neurodevelopment, Sepsis, Media and Broadcasting Twitter: @Celynkenny |
|
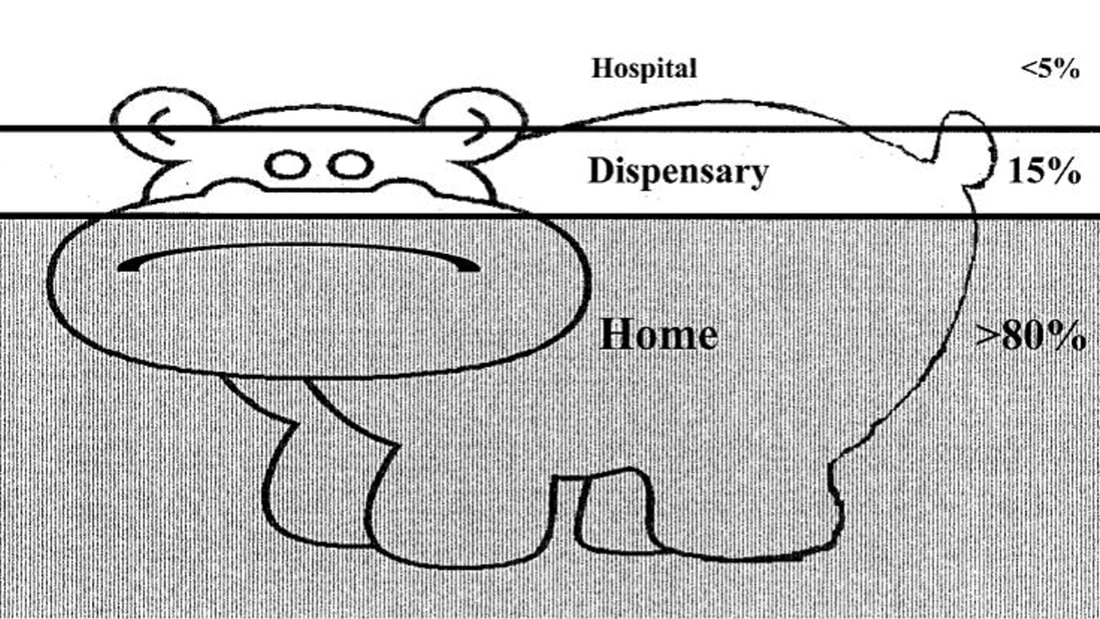
Guest Post by Dr Emily Clark The Sustainable Development Goals, launched in 2015, are ambitious. For example: "By 2030, end preventable deaths of newborns and children under 5 years of age, with all countries aiming to reduce neonatal mortality to at least as low as 12 per 1,000 live births and under-5 mortality to at least as low as 25 per 1,000 live births” This is a tough challenge we have set ourselves. Current global neonatal mortality (NMR) stands at 19/1000 live births, with under-5 mortality (U5M) at 41/1000 live births. In Madagascar, the NMR is 19/1000 live births, and the U5M 46/1000 live births (1). Note that these figures are all averages, which hides variation between regions, between rich and poor, between the educated and the illiterate (Hans Rosling has an excellent talk on this). I worked in a remote coastal region of southwest Madagascar, where there are no local data available for neonatal or child mortality as many births, and deaths, are not registered. I imagine that the statistics here would be worse than the average as communities are subject to the inverse care law: the paradox that those with the greatest need for health care have the least access. However, in terms of mortality rates, we have come a long way already. At the start of the Millennium Development Goals (MDGs) in 1990, the global NMR was 37/1000 live births (40/1000 in Madagascar), and the U5M was 93/1000 live births (160/1000 in Madagascar) (1). The Millennium Development Goals report states: “The dramatic decline in preventable child deaths over the past quarter of a century is one of the most significant achievements in human history” So what works, and what do we need to do? We know that most childhood illnesses are managed at home. This is memorably described in the case of malaria as the “ears of the hippo” – where only the minority of children are seen in a health facility. ‘‘The Ears of the Hippopotamus’’ where malaria patients are managed . . . and die. (2) How do we get children from home to the hospital? And how do we do so within a timely manner? The three delays model was devised in 1994 by Thaddeus and Maine (3). It states that the delay in a sick person receiving appropriate medical care can be broken down as follows: 1. The delay in recognition that medical help is required 2. The delay in arriving at a location where appropriate medical help can be given 3. The delay in receiving appropriate help at this location Rather than making the sick travel to the health centre, bringing health workers into the communities has demonstrated a reduction in childhood mortality. This initiative, known as Integrated Case Community Management (ICCM), targets the top causes of childhood deaths: diarrhoea, malaria, and pneumonia. If implemented globally, early treatment in the community of pneumonia in under-fives could reduce mortality by more than two-thirds. Similarly, community-based treatment of malaria could halve malaria-related mortality. Three-quarters of deaths from diarrhoea could be prevented by administration of oral rehydration solution (4). ICCM also promotes identification and treatment of malnutrition, which is observed in one-third to one-half of childhood deaths. I volunteered with Blue Ventures, a marine conservation NGO, working in remote coastal southwest Madagascar. I worked with their community health team, Safidy, which means “choice” in Malagasy. Here, it is all too easy to understand how receiving timely and appropriate medical intervention was a challenge. Health literacy was poor, transport infrastructure was sparse (relying on zebu carts, fishing pirogues, and ad hoc cars and lorries). The roads were sandy tracks, and driving to the city takes 7 hours to cover the 200km on a good day – and that was in a 4x4. Sadly, this is unaffordable to most. Poverty underlies life here. There is no money available for medicines, transport; many can simply not afford not to work for a day. As part of the Safidy programme, each village in the Blue Ventures service area has one agent communautaire (AC). These ACs, already respected women within their communities, were invited by the ICCM programme to an intensive eight-day residential training course. The training was centred around the use of a fiche, a paper-based form containing a series of questions which guide the ACs through key symptoms to aid diagnosis, and the “danger signs” of serious illness. These danger signs should prompt immediate treatment, as specified by the fiche, and referral to a health centre. The fiche guides ACs in providing safety net advice and follow up arrangements. The ACs also educate communities regarding public health measures, such as promotion of exclusive breastfeeding, and immunisations. ACs are provided with key items of equipment, such as rapid diagnostic tests for malaria, a measuring strip for mid-upper arm circumference for assessment of malnutrition, and a one-minute timer for measuring respiratory rate. Essential medicines are also provided, including oral rehydration solution and zinc, antibiotics for pneumonia, and anti-malarials. When a child falls ill, it is easy for the family to ask the AC within their own village for advice. The AC is able to assess and triage the child, and decide, using the fiche, what treatment is required. For example, a child presenting with a cough may well have pneumonia; the AC should then check for fever, and measure the respiratory rate. If the respiratory rate is raised, this should prompt antibiotic treatment and referral to a health centre. If there are no danger signs present, then the AC can provide a course of antibiotics and appropriate follow up advice. All the ACs are literate, however, they have had very limited education at school. Yet, these women perform the same job that we do, as a multi-disciplinary team, in the Children’s Assessment Unit. They are simply phenomenal. It is a lot to learn, and so, together with a local ICCM trainer, the Safidy team arranged for two study days for the newly-trained ACs. The focus was on role play rather than theory. Many of the ACs had brought their children along to the training and so they made for excellent “patients”, and so we witnessed some Oscar-worthy performances! Each AC received feedback on their performance: what went well, what could be improved next time. The ACs will now spend time working under direct supervision from nurses and midwives at local health facilities, before being approved to work independently within their communities. We hope that the success of ICCM in other countries can be replicated in this little corner of Madagascar. One AC measures a young actor’s respiratory rate using a specially-designed timer A trainer demonstrates assessment for pedal oedema; a danger sign that should prompt referral to a health centre Further reading For more reading on the Sustainable Development Goals: http://www.un.org/sustainabledevelopment/sustainable-development-goals/ The WHO have produced a report on the evidence for ICCM, available here: http://www.who.int/maternal_child_adolescent/documents/iccm_service_access/en/ To see data being brought to life, I would advise watching Hans Rosling – starting here: https://www.ted.com/talks/hans_rosling_shows_the_best_stats_you_ve_ever_seen ICCM complements the WHO programme Integrated Management of Childhood Illness (IMCI) which aims to improve the quality of care available to patients at health facilities. A recent Multi-Country Evaluation has demonstrated that quality of care is improved, resulting in a reduced childhood mortality. It has demonstrated cost-effectiveness, as earlier and correct treatment saves money. http://www.who.int/maternal_child_adolescent/topics/child/imci/en/ For more information regarding Blue Ventures’ community health programme, Safidy: https://blueventures.org/conservation/community-health/ References:
(1) All data from the World Bank, http://www.worldbank.org/ Accessed 20.03.2018 (2) The Intolerable Burden of Malaria: A New Look at the Numbers: Supplement to Volume 64(1) of the American Journal of Tropical Medicine and Hygiene. Breman JG, Egan A, Keusch GT, editors. Northbrook (IL): American Society of Tropical Medicine and Hygiene; 2001 Jan. (3) Thaddeus S, Maine D. Too far to walk: maternal mortality in context. Soc Sci Med. 1994 Apr;38(8):1091–110. http://dx.doi.org/10.1016/0277-9536(94)90226-7 pmid: 8042057 (4) WHO/UNICEF JOINT STATEMENT Integrated Community Case Management (iCCM). United Nations Children’s Fund. 2012
0 Comments
As a Paediatrician I think we play a vitally important role in Public Health, we have the ability to make a significant difference with every contact we have with children and young people, therefore I was excited to attend the Public Health Wales Conference in October. It provided an opportunity to keep up to date with all aspects of Public Health as well as focus in on paediatric specific topics, such as adverse childhood events, the venue was fantastic and with Michael Sheen making a keynote presentation what was not to love?! The start to day 1 was nothing short of inspirational, a montage of pictures detailing the history of Public Health in Wales and significant events in history, such as devolving power over health, was accompanied by a harp and a flashmob choir popping up in the audience culminating in a local school choir taking to the stage, it was breath taking. After an impressive start the audience heard from Rebecca Evans, Minister for Social Services and Public health, who updated us on the progress which Wales had made within Public health. The next speaker Dr Christoph Hamelmann, Head of the World Health Organisation Europe office for Investment in Health and Development, spread the net wider and discussed more global issues and reiterated the importance in looking beyond your own borders in Public Health spheres. I was pleased to learn that the ‘Well being of future generations act” really is leading the way within the WHO. We wrapped up before lunch with a keynote on Climate change, followed by a discussion panel exploring air pollution and how we can build a sustainable future. The afternoon sessions on day one were split into ‘Spotlight sessions’ there were many of these going on at the same time and the topics which you could choose from were diverse. I attended one entitled “Mindfulness for wellbeing: Evidence and Practise” The science behind mindfulness was discussed briefly, demonstrating the activation of the pre-frontal cortex when being mindful. Children who are naturally high in mindfulness react less strongly and have better emotional regulation. It was interesting to see demonstrated that by using mindfulness techniques with school aged children you can shift them into individuals with high mindfulness. After the training these children had a significant decrease in the intensity of their reactions to angry faces. Mindfulness has an enormous potential for development within education, as within other areas, but it important that the training is ongoing and children learn to use it within everyday life. Mindfulness, growth mindset and metacognition are surrounding feature of the new curriculum being developed in Wales and has the opportunity to vastly improve the outcomes in mental health for this generation of children. My spotlight session was fantastic, but I had significant spotlight session envy as a college attended a Lego workshop based on driving improvement through the value chain and got to use LEGO to demonstrate visually resilience and improvements – she got to play with LEGO and call it work! (on a side note you can train to deliver LEGO sessions and this could be your job!)
Day 1 ended with a chaired Brexit Debate. The views from the panel were interesting and the uncertainty regarding the exit plans are already causing problems for Public Health initiatives within Wales. The panel presented reasoning that it doesn’t matter what side you were on when voting took place, we need to overcome this and work together to move forward. Wales have already done some of the ground work with how to respond. Brexit is currently overwhelming all of UK politics and other important issues are being neglected because of this focus. But on the other side of the coin, and attempting to be a glass half full type of person, Brexit is a huge opportunity to have ‘No more excuses’ and reduce inequalities. We need to change our mindset on Brexit, accept that it is currently happening and focus on the positives which we can derive from it. Day 2 started by hearing from Dr Frank Atherton who is Chief Medical Officer for Wales and a person I will never get bored of hearing speak. He attended WPS last Autumn and delivered an engaging Keynote there, and as a Welsh Clinical Leadership Fellow we have been in the privileged position to meet him on several occasions. He presented that we should celebrate our Public Health successes (Hepatitis C, Future generations act, reduction in smoking rates) but also recognise that we still have a long way to go. Inequalities still exist and are widening. Moving forward we need to focus on prevention with improved outcomes and ensure sustainability. But because a long term view is not easy to fit into political cycles it is hard to engage managers with this viewpoint. Dr Atherton concluded that we are on the right track and need to continue to engage the public and sustain ongoing developments in Prudent Health Care. Dr Chrissie Pickin followed on from Frank Atherton and presented an engaging talk entitled “Understanding people’s choices and how to influence them”. She started by noting that Health issues are complex and for every complex problem there is a straightforward, easy to implement, wrong solution. Providing education is an obvious solution because the assumption is that people would not deliberately harm themselves but a knowledge gap is rarely the reason behind the behaviour. She gave some top tips to influence people’s choices.
Having learnt about how to influence people’s choices it was fitting that the next speaker, Richard Chataway delivered a talk on Social Marketing and Communication Science. Because we have a better understanding of what drives behaviour change as well as advances in technology social marketing has significantly changed. Richard Chataway presented, amongst other topics, a public health initiate undertaken in Australia, his team wanted to reduce smoking rates. When quitting smoking the motivation is there, the knowledge is there but people need support. He launched My Quit Buddy, an app which provided daily progress tracking, distraction techniques and motivational messages. This was an incredibly successful campaign and the app has had wide uptake. He also explored the use of technology within research into changing behaviours. With the introduction in artificial intelligence it is possible to pre-test communications such as an advertising campaign, to understand it people will find it motivating at a subconscious level this can remove the test and learn element of marketing which will make it more effective, quicker. He again reiterated that in order to find a solution it is important to understand the behaviour and design a solution around it. A panel discussion followed this. After a short break, there were more ‘Spotlight sessions’ with lunch in the middle. There were again many topics to choose from. I attended “Tackling Adverse Childhood Experiences” It is known that if a young person experiences 4 events they are 15x more likely to commit violence, 14x more likely to experience violence and 20x more likely to be in prison than the general population. We need to break the generational cycle and make a social movement for change looking at the root causes and take a psychological approach to tackle these. The impact of breaking the generational cycle is huge, 47% of adults have experience 1 adverse event. The second of my ‘spotlight sessions’, after lunch was “The good, the bad and the social: Two sides of social media” Social media is more addictive than smoking or alcohol, 10 million photos are uploaded to Facebook every hour. It can be both positive and negative the challenge comes with harnessing the positives while mitigating the negatives. Instagram is cited as the most negative with associations to negative body image as well as anxiety and cyber bullying. There was a lot of discussion about where the responsibility lies for managing social media for children and young people. It was felt that this was not just the responsibility of parents, social media itself needs to take some responsibility. The conference closed with Michael Sheen discussing “Building on our cultural strengths: Supporting communities.” As expected Michael Sheen was an engaging and well informed speaker. His message began with the understanding the if you want different outcomes you have to fundamentally change what you do. He outlines inequality as a significant problem, the less you have the more you have to pay for it. If we want families to drive themselves up socially then we need to look at the weight of debt which they have. We have a benefit within Wales as we have a strong community spirit and have held onto our identity and language. As a Public Health team we need to support our communities to be as healthy and sustainable as possible, we need to provide space where communities can come together and shift the power into the grass roots. His concluding statement is worth recognition and highlights a positive to finish a highly engaging conference. “One who has health has hope, and one who has hope, has everything” (Originally a proverb I think!) Once again, I tweeted through the conference and these can be found on my twitter feed from these dates. Public Health is an important topic which is extremely relevant within Paediatrics and the selection of work presented during this conference leaves me in no doubt that Wales really is leading the way. |
Editors
Dr Annabel Greenwood Categories
All
|









 RSS Feed
RSS Feed
