|
Dr Tom Cromarty Editor Interests: Paediatric Emergency Medicine, Medical Engagement and Leadership, Simulation, Quality Improvement, Research Twitter: @Tomcromarty |
Welsh Research and Education Network
WREN BlogHot topics in research and medical education, in Wales and beyond
Dr Celyn Kenny Editor Interests: Neonates, Neurodevelopment, Sepsis, Media and Broadcasting Twitter: @Celynkenny |
|
Wednesday 29th November 2017 Summary Newsletter and Projects Information By Chris Course The Welsh Research and Eduction Network (WREN) Autumn Study Day took place at the Princess of Wales Hospital, Bridgend on 29th November 2017. We had a really good turnout with lots of trainees keen to learn more about research, aided by the morning educational sessions (see further information below). Following this, there were updates on the current WREN project portfolio, with completed projects on audiology follow-up after meningitis being presented by Fiona Astill, and Siwan Lloyd presenting her work on the referral process for developmental delay. Qumrun Nahar presented her preliminary work on the use of botox for spasticity in Pembrokeshire, with plans to expand the project to other health boards in Wales. Full details of the project results will be published on our website shortly. With one large-scale project still ongoing, and two more planned for the start of 2018, there’s still lots going on within the network to get involved with!
Additionally, the new WREN Blog (www.wrenpaediatrics.com/blog) was launched last month, and is being edited by Rebecca Broomfield and Annabel Greenwood. They will be publishing on the first of each month on a range topics, including conference reports, critical appraisal and current research happening in Wales now. They are looking for contributors too, so if you have something to share or a topic you’d love to write about, please get in touch. Details of the WREN projects and their project leads, with contact details, are below. We will be disseminating these projects amongst the units, but if you would like to get involved in any of the projects in WREN’s current portfolio, please contact the project leads (details below). If you have an idea for a project you would like to develop with WREN’s help, please contact either myself or Siwan Lloyd via our website or using the details at the top of this newsletter. The next WREN study day is planned for May 2018 (confirmed date to follow), and we hope that you will be able to join us for another stimulating and thought-provoking study day, building on from the success of the last! Education The morning educational sessions were focussed on the importance of good research practice, with Health and Care Research Wales coming to give an update on Good Clinical Practice (GCP) for paediatrics. The added complexities of research for the paediatric population were highlighted, as well as the robust nature of research methodology to ensure valid results. The workshop received excellent feedback, and all attendees received a certificate for their portfolios. This was followed by Kate Burke and David Gallagher coming to share their experiences of taking time out from clinical training to undertake a PhD. The highs and the lows of their journeys were illuminating, and their varied experiences of the opportunities on offer, like experiencing a European neonatal units way of working, plus the ability to develop new lab skills, demonstrated the gains to be had. The realities of thesis writing were made plain though, so there’s always a flip-side! Thanks to our our speakers for an excellent morning educational session. Ongoing Projects: Project Title: ‘Antibiotic use on the post-natal wards.’ Project Lead: Zoe Howard, ST5 Royal Glamorgan [email protected] (and Annabel Greenwood ST3, UHW [email protected] and Chris Course, ST4 UHW) Description: NICE guidance on the management of suspected early-onset neonatal sepsis has existed for several years, however management appears to vary across units throughout Wales. A prospective audit of infants started on antibiotics for suspected sepsis post-delivery is underway for units across Wales. A comparison of local unit guidelines across Wales is also a part of this project. This project has so far completed 4 months of data collection, and is planning on completing a further two months before starting data analysis. So far data on more than 200 infants has been gathered. Upcoming Projects: Project Title: ‘Head injuries on the postnatal wards’ Project Lead: Siwan Lloyd, ST3 Noah's Ark Children's Hospital for Wales [email protected] Description: A pilot study at UHW has demonstrated that infants being accidentally dropped on the postnatal ward is not an uncommon occurrence, however their management and level of investigation following injury was very variable. Following on from this, an all Wales study is planned to determine the incidence, risk factors and management used, with the aim of producing a best practice guideline for these infants and their parents. Project Title: ‘Re-audit of the Management of Respiratory Distress Syndrome in Preterm Infants’ Project Lead: Chris Course, ST4 Noah's Ark Children's Hospital for Wales [email protected] Description: Following the initial audit in 2014/2015 by WREN, a Wales Neonatal Network guideline was introduced for the Management of RDS in Preterm Infants in June 2016. The re-audit is planned to commence in March 2018 and will run for six months to assess how the new national guideline has affected patient care.
1 Comment
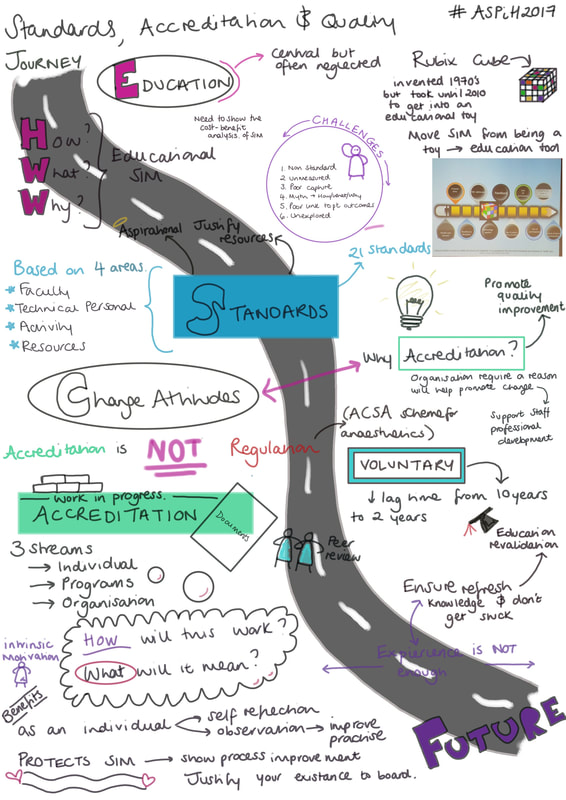
 Association for Simulated Practise in Healthcare (ASPiH), 6th – 8th November 2017, Telford International Centre By Rebecca Broomfield As a part of my Clinical Leadership Fellow year I am focusing on the evaluation of simulation as a teaching technique, attempting to relate this to improved patient safety and improved patient outcomes. Anybody who knows me knows that I love a simulated scenario as a teaching session, it’s not everybody’s cup of tea but it really fantastic opportunity to learn. I therefore jumped at the chance to attend the ASPiH conference. I started by attending a pre-conference workshop session based on Evaluation of Simulation. I was actually unaware that pre-conference workshops happened. A lot of big conferences have a day prior to the main event which they run focus groups or workshops that people can attend to be taught and explore ideas with like minded others. My workshop covered a lot of educational theory behind simulation and how you can use this to evaluate your simulation sessions. Key learning points included the fact that a poor evaluation undermines the development of new approaches. The evaluation itself is “a systematic acquisition and assessment of info to provide useful feedback about some [object]”, therefore while evaluation of the session is often an afterthought and a quick Likert score which nobody reads or bothers to fill in correctly, it really should be an important part of the structure of the simulation session. We also discussed how to structure your evaluation and a way to form a measurable outcome. The actual conference kicked off on the Tuesday morning. There were key note sessions delivered at different points in the day and there were split sessions with a choice of what to attend between these. The keynotes were all interesting a relevant to current trends in simulation. Cherrie Evan’s talk on delivering simulation based education in Africa was an eye opener and inspiring to see how correctly administered simulation can really make a significant difference in patient safety and improve outcomes. Her work was through an organisation called Jhpiego and focuses on the safety of a mother and newborn at delivery. Dr Gabriel Reedy delivered a session on the educational theory behind education, which is particularly relevant to my project. All the keynotes can be found at: http://www.youtube.com/playlist?list=PLzm6Ad9XIwxmnblhwSbEcjceDNpUFW1iu - I’d also recommend watching Dr Al Ross’ talk on Resilience within healthcare if like me you’ve become a bit disillusioned with the term resilience and its meaning. In between the keynotes there was so much going on, it was almost overwhelming. Sessions ran throughout the day with presentations about many different aspects of simulation from setting up in-situ simulations with an emergency department, evaluation of simulation sessions and development of simulations focusing on wellbeing and resilience. The sponsors were around with lots of new technology and we got to play with all the new simulation models. There is a particularly interesting baby and child model which is amazingly lifelike and provokes significant emotion (I automatically checked the veins on this model immediately after picking it up!) I also got to observe a session using a interactive tent to have a projected environment in which to run a simulation. The situation that I observed was a building site with an injured builder. The walls were displaying images of a new housing estate and there were building site noises being played throughout. The tent feeds into the educational theory of distributed cognition suggesting that we need to be investing cognitive power into the technology as well as the people.
ASPiH is working hard to provide a standardised quality simulation teaching nationwide and as such they have developed their standards documents which can be found here: http://aspih.org.uk/standards-framework-for-sbe/. These outline the standard expectations for running a good simulation education program. It is looking into developing an accreditation system in order to promote good quality simulation. We know that simulation teaching is good, we now need to prove it and regulate its delivery in order to standardise experiences. I am even more excited about simulation teaching and its huge potential since attending this conference. I tweeted throughout the days including sketchnotes of some of the sessions I attended, if you are interested in these they are on my twitter feed for the conference dates. I am planning on attending the Paediatric specific International Pediatric Simulation Society (IPSS) conference during May in Amsterdam, if anybody fancies joining me you’d be welcome. If you want more information on ASPiH then visit their website here: http://aspih.org.uk/ As a Paediatrician I think we play a vitally important role in Public Health, we have the ability to make a significant difference with every contact we have with children and young people, therefore I was excited to attend the Public Health Wales Conference in October. It provided an opportunity to keep up to date with all aspects of Public Health as well as focus in on paediatric specific topics, such as adverse childhood events, the venue was fantastic and with Michael Sheen making a keynote presentation what was not to love?! The start to day 1 was nothing short of inspirational, a montage of pictures detailing the history of Public Health in Wales and significant events in history, such as devolving power over health, was accompanied by a harp and a flashmob choir popping up in the audience culminating in a local school choir taking to the stage, it was breath taking. After an impressive start the audience heard from Rebecca Evans, Minister for Social Services and Public health, who updated us on the progress which Wales had made within Public health. The next speaker Dr Christoph Hamelmann, Head of the World Health Organisation Europe office for Investment in Health and Development, spread the net wider and discussed more global issues and reiterated the importance in looking beyond your own borders in Public Health spheres. I was pleased to learn that the ‘Well being of future generations act” really is leading the way within the WHO. We wrapped up before lunch with a keynote on Climate change, followed by a discussion panel exploring air pollution and how we can build a sustainable future. The afternoon sessions on day one were split into ‘Spotlight sessions’ there were many of these going on at the same time and the topics which you could choose from were diverse. I attended one entitled “Mindfulness for wellbeing: Evidence and Practise” The science behind mindfulness was discussed briefly, demonstrating the activation of the pre-frontal cortex when being mindful. Children who are naturally high in mindfulness react less strongly and have better emotional regulation. It was interesting to see demonstrated that by using mindfulness techniques with school aged children you can shift them into individuals with high mindfulness. After the training these children had a significant decrease in the intensity of their reactions to angry faces. Mindfulness has an enormous potential for development within education, as within other areas, but it important that the training is ongoing and children learn to use it within everyday life. Mindfulness, growth mindset and metacognition are surrounding feature of the new curriculum being developed in Wales and has the opportunity to vastly improve the outcomes in mental health for this generation of children. My spotlight session was fantastic, but I had significant spotlight session envy as a college attended a Lego workshop based on driving improvement through the value chain and got to use LEGO to demonstrate visually resilience and improvements – she got to play with LEGO and call it work! (on a side note you can train to deliver LEGO sessions and this could be your job!)
Day 1 ended with a chaired Brexit Debate. The views from the panel were interesting and the uncertainty regarding the exit plans are already causing problems for Public Health initiatives within Wales. The panel presented reasoning that it doesn’t matter what side you were on when voting took place, we need to overcome this and work together to move forward. Wales have already done some of the ground work with how to respond. Brexit is currently overwhelming all of UK politics and other important issues are being neglected because of this focus. But on the other side of the coin, and attempting to be a glass half full type of person, Brexit is a huge opportunity to have ‘No more excuses’ and reduce inequalities. We need to change our mindset on Brexit, accept that it is currently happening and focus on the positives which we can derive from it. Day 2 started by hearing from Dr Frank Atherton who is Chief Medical Officer for Wales and a person I will never get bored of hearing speak. He attended WPS last Autumn and delivered an engaging Keynote there, and as a Welsh Clinical Leadership Fellow we have been in the privileged position to meet him on several occasions. He presented that we should celebrate our Public Health successes (Hepatitis C, Future generations act, reduction in smoking rates) but also recognise that we still have a long way to go. Inequalities still exist and are widening. Moving forward we need to focus on prevention with improved outcomes and ensure sustainability. But because a long term view is not easy to fit into political cycles it is hard to engage managers with this viewpoint. Dr Atherton concluded that we are on the right track and need to continue to engage the public and sustain ongoing developments in Prudent Health Care. Dr Chrissie Pickin followed on from Frank Atherton and presented an engaging talk entitled “Understanding people’s choices and how to influence them”. She started by noting that Health issues are complex and for every complex problem there is a straightforward, easy to implement, wrong solution. Providing education is an obvious solution because the assumption is that people would not deliberately harm themselves but a knowledge gap is rarely the reason behind the behaviour. She gave some top tips to influence people’s choices.
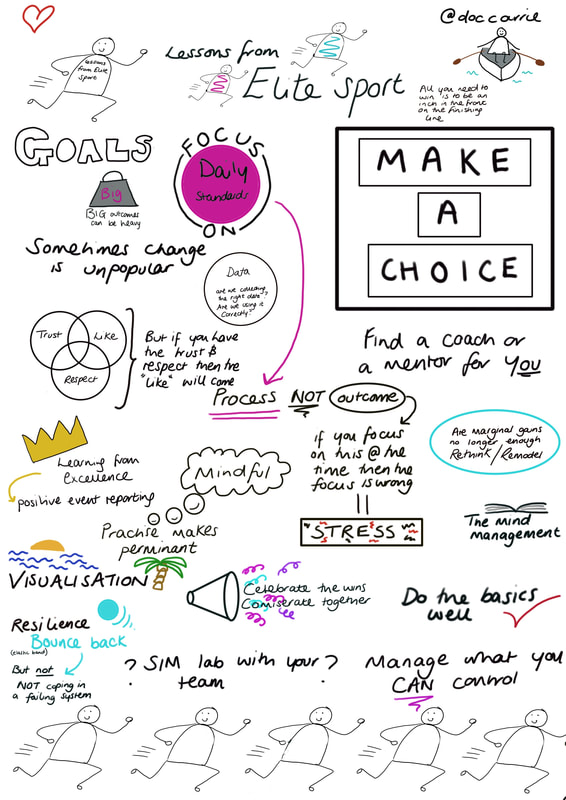
Having learnt about how to influence people’s choices it was fitting that the next speaker, Richard Chataway delivered a talk on Social Marketing and Communication Science. Because we have a better understanding of what drives behaviour change as well as advances in technology social marketing has significantly changed. Richard Chataway presented, amongst other topics, a public health initiate undertaken in Australia, his team wanted to reduce smoking rates. When quitting smoking the motivation is there, the knowledge is there but people need support. He launched My Quit Buddy, an app which provided daily progress tracking, distraction techniques and motivational messages. This was an incredibly successful campaign and the app has had wide uptake. He also explored the use of technology within research into changing behaviours. With the introduction in artificial intelligence it is possible to pre-test communications such as an advertising campaign, to understand it people will find it motivating at a subconscious level this can remove the test and learn element of marketing which will make it more effective, quicker. He again reiterated that in order to find a solution it is important to understand the behaviour and design a solution around it. A panel discussion followed this. After a short break, there were more ‘Spotlight sessions’ with lunch in the middle. There were again many topics to choose from. I attended “Tackling Adverse Childhood Experiences” It is known that if a young person experiences 4 events they are 15x more likely to commit violence, 14x more likely to experience violence and 20x more likely to be in prison than the general population. We need to break the generational cycle and make a social movement for change looking at the root causes and take a psychological approach to tackle these. The impact of breaking the generational cycle is huge, 47% of adults have experience 1 adverse event. The second of my ‘spotlight sessions’, after lunch was “The good, the bad and the social: Two sides of social media” Social media is more addictive than smoking or alcohol, 10 million photos are uploaded to Facebook every hour. It can be both positive and negative the challenge comes with harnessing the positives while mitigating the negatives. Instagram is cited as the most negative with associations to negative body image as well as anxiety and cyber bullying. There was a lot of discussion about where the responsibility lies for managing social media for children and young people. It was felt that this was not just the responsibility of parents, social media itself needs to take some responsibility. The conference closed with Michael Sheen discussing “Building on our cultural strengths: Supporting communities.” As expected Michael Sheen was an engaging and well informed speaker. His message began with the understanding the if you want different outcomes you have to fundamentally change what you do. He outlines inequality as a significant problem, the less you have the more you have to pay for it. If we want families to drive themselves up socially then we need to look at the weight of debt which they have. We have a benefit within Wales as we have a strong community spirit and have held onto our identity and language. As a Public Health team we need to support our communities to be as healthy and sustainable as possible, we need to provide space where communities can come together and shift the power into the grass roots. His concluding statement is worth recognition and highlights a positive to finish a highly engaging conference. “One who has health has hope, and one who has hope, has everything” (Originally a proverb I think!) Once again, I tweeted through the conference and these can be found on my twitter feed from these dates. Public Health is an important topic which is extremely relevant within Paediatrics and the selection of work presented during this conference leaves me in no doubt that Wales really is leading the way. Leaders in Healthcare Conference 30th October – 1st November 2017, ACC Liverpool By Rebecca Broomfield I am currently taking a year out from the Paediatric training program and doing a Clinical Leadership Fellows placement through the Wales deanery. As a part of this year we come under the umbrella of the Faculty of Medical Leadership and Management (FMLM), it was under this disguise we managed to sneak ourselves into the FMLM’s annual conference "Leaders in Healthcare". I went to this conference with an initially pessimistic outlook. I truly believed that a lot of the information provided would be over my head, in a language that I didn’t understand, from managers who were slightly out of touch. I am humble enough to eat my own thoughts and I would thoroughly recommend everybody tries to attend an FMLM conference at some point in their career, indulge me and read on to discover why! As per conference structure, which I am becoming more and more familiar with, Day 1 began with a welcome – another choir, (starting to think this is a new trend .... perhaps someone could do a study?) followed by a Key note speaker. Seriously, this was an impressive start. We heard from Nicky Moffat in a keynote entitled “Leadership is everyone’s business” Nicky Moffat has a background in the military and spoke about the importance of not buying in people for leadership roles but investing in people and growing them up from within. She voiced an important message of inclusion; that every person has a role to play, as a leader your role is to value these differences and figure out how to make them work. You do not have to be able to do everything, but you do have a responsibility to those who you lead to dedicate time to your own personal development. You set the tone, so make sure that you lead your way. She was inspirational to listen to and it was particularly interesting to hear from somebody whose career was outside of medicine but was experienced in a structured, high-pressured environment. After a brief pause for coffee, we split into smaller group sessions. I went for a workshop entitled “Joy in work”. It was run by Henry Stewart, a man who introduced himself as “Chief happiness officer”, which I love, who wouldn’t want that to be their job title??! He runs the Happy company, which has been listed as one of the 20 best workplaces in the UK for five successive years (www.happy.co.uk). Henry Stewart has also written “The Happy Manifesto” a book that has made it onto my Christmas wish list (along with many others from this conference alone.) The company motto is “Don’t tell when you can ask” He has identified that people work better when they are challenged and given freedom. As a manager we should be enabling people to innovate, and rather than focusing on weaknesses we should develop our strengths. Mistakes should be celebrated and, within the boundaries of clear principles and targets, team members should be given freedom and ownership of projects. The style of the session was relaxed, he actively encouraged participation, and provided a significantly different perspective on workplace than my experience of the NHS. Lunch provided an opportunity to network with other conference attendees. There was a wide range of people present, many with backgrounds in significant leadership positions within the NHS. My after lunch session focused on collaboration across barriers and introduced me to the concept of Compassionate Leadership, which will be a blog post for the future. I didn’t want to stick to hearing from people with leadership roles within the NHS, so I headed to a second afternoon session delivered by Carrie Thomas, who herself is an ST4 in emergency medicine, but was delivering a session on how we can learn lessons from elite sport. She directed the audience to focus on the daily standards, looking at the processes rather than focusing on the outcome. She advised learning from excellence, managing what you are able to control and utilising visualisation to drive you forwards. Remember that you are a team and it is vitally important to work together, not only should you commiserate together but you should celebrate the wins. Day 1 ended with an incredibly passionate and moving talk from Gulwali Passarlay (his book “The Lightless Sky” has also made it onto my wish list!). Guwali started with a thank you and a reminder not to forget the little things you do as clinicians daily as they are the important things. He spoke about his incredible journey as a child refugee travelling alone from Afghanistan across 12 countries, to end up in Britain, go to university and carry the Olympic torch in 2012. It served as an acute reminder of our privileges. His story was about overcoming adversity and never giving up. He reminded his audience that having an experience was one thing, but how you used that experience was another; you have a choice. At the start of day 2 Dr Bruce Keogh, hopefully an man who needs no introduction, delivered the opening keynote. He started by stating that we do not want to loose our NHS by mistake and received a standing ovation at the end of his talk. He outlined the history of the NHS and spoke about innovation. I’m not entirely sure that I agreed with some of what he said, but that is probably best left out of this blog for fear of entering a political minefield that I am unable to control or step back from. He did make a very valid point however, stating that people do not fear change, they fear loss. I will be taking this forward as a part of this year, and my future career. An important role as a leader is to engage people, bring them with us, inspire them to innovate and together we will be able to make a difference. As per day 1, day 2 then broke into smaller group sessions. I attended a resilience workshop. This started by recommending everybody watch ‘Inside Out’, which already had me engaged and listening. The workshop ran through 4 stages of coping and looked at each of these. They explained that resilience found ways to bypass stages, and therefore you progress through these stages quicker, or even skip some stages when faced with conflict or a challenging situation. The focus on the ability to define the problem, which would enable you to employ the correct solution. For example, it is important to be direct in complex situations. Building resilience is based on 4 key pillars; confidence, social support, purposefulness and adaptability. They encouraged assessing your own resilience, a tool to do this can be found here; www.robertsoncooper.com/iresilience/ and focusing on one weakness to improve. It was an interesting session, and do now go and watch ‘Inside Out’! After lunch I focused on 'Changing Culture'. Culture is important within a workplace because it impacts the mood and atmosphere which in turn affects performance. Leadership is about gestures and choices which we make all of the time and these influence the culture within our teams. Culture itself cannot be managed, it is a behaviour pattern which becomes established and over time this is reinforced and amplified by visible artefacts. Changing culture is what we are ultimately trying to achieve with our quality improvement projects. Small gestures can create tipping points which is known as the butterfly effect. Within culture change, the leader is in charge but not in control, this is complexity thinking which involves non linear relationships which cannot be predicted. However, machine thinking is the predominant discourse in the NHS; the NHS can be managed and the leader has complete control. The down sides to machine thinking is that everything falls to the leader, participants and team members are passive which leads to significant amount of stress and pressure. A switch from machine thinking to complexity thinking will change the culture. It is hard but as clinical leaders we should be brave! Make that change, a small shift can have a much wider impact. All of us are leaders and we need to recognise this. The final small group session I attended was on coaching – I am exploring this more on a personal level and will during, the course of the year, write a blog solely focused on this theme.
The Leaders in Healthcare conference closed with a keynote from Deborah Rowland: “How to lead mindful change” The most important message I will take from her session is that good leadership starts with knowing yourself. Invest in yourself as a leader, understand your strengths and weaknesses and recognise them without judgement. When you have spotted something you are able to change it, if you don’t look for it and recognise it, then you cannot. Her four key messages for developing your own leadership style were: Perceiving (tuning into the system), Noticing (staying present), Integrating (all aspects, including difficulty) and Choosing (respond, don’t react). To run through all of these points would take a blog post in it’s own right so instead I will direct you to her book, ‘Still Moving’ which is a challenging but useful read. In conclusion, despite my initial reservations, the Leaders in Healthcare conference was an extremely simulating and enjoyable two days. I never felt during sessions that voicing my opinion was not as valid as the opinion of somebody with significantly more leadership experience than myself. The conference has inspired me to continue to develop myself as a leader, and to first reflect on my own skills and weaknesses which will enable me to be better equipped to help guide the NHS through the challenging times ahead. I would encourage everybody to take a look at the FMLM website and available courses and opportunities www.fmlm.ac.uk
Once randomized, children will be followed up over a 28-day period, with telephone contact at 7, 14 and 21 days, and a face-to-face consultation at 28 days. Parents are also keeping a daily symptom diary to monitor their child’s progress, as well as filling in wellbeing questionnaires at the contact times. Pre- and post-treatment nasoparyngeal and saliva swabs are being taken to analyse bacterial resistance patterns.
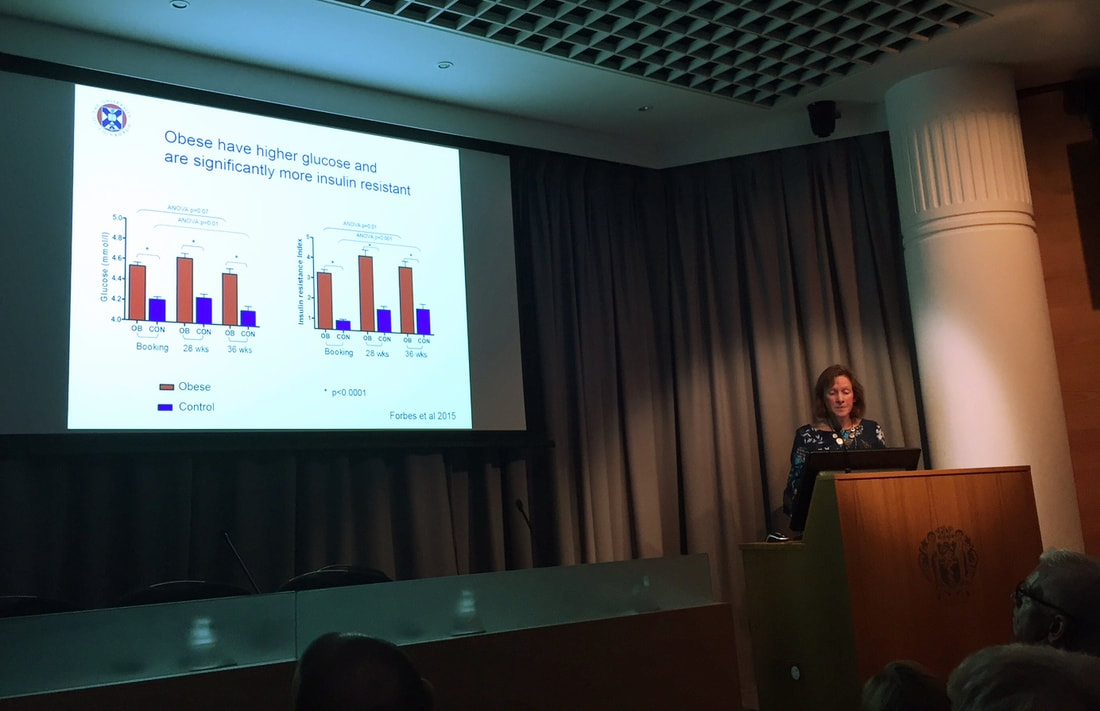
CAP-IT is planned to be recruiting over the next two winters with a target cohort of around 2,500 children, so is still in its early phases. It’s one of the first major trials being run out of the new Children and Young People’s Research Unit, based at the Noah’s Ark Children’s Hospital for Wales. For anyone that is interested and wants to know more, or even get involved, please get in touch with WREN and we can point you in the right direction! Links to the protocol and website are included at the bottom of the article. So, hopefully in a few years, we may understand this common condition a little better, but more importantly, the best way to treat it and ensure that treatment will continue working for the generations to come. CAP-IT: Efficacy, safety and impact on antimicrobial resistance of duration and dose of amoxicillin treatment for young children with Community-Acquired Pneumonia (CAP): A randomized controlled trial. www.capitstudy.org.uk http://www.ctu.mrc.ac.uk/our_research/research_areas/other_conditions/studies/cap_it/ 9th November 2017, Royal Society of Medicine, London By Chris Course On 9th November, the Neonatal Society held their Autumn Meeting at the Royal Society of Medicine in London. The program included oral presentations of submitted abstracts as well as invited guest speakers. There were a variety of topics covered, from studies looking at postnatal dexamethasone use upregulating surfactant proteins in preterm lamb models, surgical outcomes of preterm infants with congenital diaphragmatic hernia over a twenty-year period, increasing demands on neonatal unit for management of hypoglycaemia and breastmilk exposure influencing preterm brain development. The Widdowson lecture was given by Professor Pierre Gressens of King’s College and concerned the genomics of preterm brain injury. To be honest, some of the technicalities of the science and molecular pathways went a bit over my head, but there seemed to be some promising preliminary results on upregulating pro-repair inflammatory pathways and suppressing the damaging and immunomodulatory pathways by using tiny engineered pieces of DNA to protect the preterm brain’s white matter. Might seem a bit removed from clinical practice now, and seemed to be still a way from trials in human subjects, but then again, in a decade who knows what we’ll be doing on the wards! The keynote lecture came from Professor Rebecca Reynolds of Edinburgh University, who gave a fascinating talk on maternal health determining offspring life-course outcome. She went through data showing that it had been identified in the 1960’s that areas with high infant mortality ratios at the turn of the last century, went on to become areas with high rates of cardiovascular deaths in later life. Over the years, various studies have been conducted looking at the fetal programming effects of raised cortisol (secondary to maternal stress) reprogramming the fetal hypothalamo-pituitary-adrenal axis, and raised BMI/poor maternal diet/lifestyle leading to impaired insulin sensitivity in the fetus. Cohorts have been followed-up which show these infants have higher rates of type 2 diabetes and poorer neurodevelopmental outcomes/behavioural problems. There’s also a cohort of mothers in Finland that’s been followed up based on the amount of liquorice they consume…. Might seem odd, but apparently, it’s a popular snack in Finland, but suppresses an enzyme in the placenta that prevents too much cortisol passing into the fetus. It really highlighted how what we do in early life, and even before conception, can affect us for the rest of our lives! It did however also make me aware that in our role as paediatricians/neonatologists we have an opportunity to change long-term health for the better too. For anyone who hasn’t been to the Royal Society of Medicine, it’s a suitably impressive venue (befitting the name really) just behind Oxford Street, which was perfect for a leisurely lunch and a spot of early Christmas shopping during the society’s business meeting. And the day was rounded off with a drinks reception – what’s not to love! The day really brought home how diverse the neonatal research world is, and how much work is going on to try and improve understanding of physiology, diseases and develop new treatments. The Neonatal Society hold three meetings a year. The Autumn and Spring meetings are one-day, held in London, are free to attend and don’t require prior registration. The Summer meeting changes location around the UK (and sometimes ventures into Europe), with next year’s being held in Dublin in June. Abstracts are invited to be submitted for all the meetings, and are a great opportunity to get projects presented at a high-quality, national meeting – good for the CV/portfolio! Additionally, once you have presented at a society meeting, you are eligible to apply for membership.
For more information, check out www.neonatalsociety.ac.uk St Brides Hotel, Saundersfoot, Friday 10th November 2017 Hosted by Glangwili General Hospital & Bronglais Hospital By Annabel Greenwood This Autumn’s WPS meeting took place in the absolutely stunning location of St Brides Hotel in the picturesque seaside town Saundersfoot. Nestled in the clifftop, overlooking the breath-taking rugged Welsh coastline, it provided the perfect backdrop for an invigorating day of presentations, discussions and networking. The day began with the invitation lecture from the esteemed Dr Trevor Brown, Consultant Paediatric Allergist at Ulster Hospital, on cow’s milk allergy (formerly cow’s milk protein allergy). Ever a diagnostic and management paradox for GPs and general paediatricians, this in-depth discussion covering IgE verus non-IgE mediated reactions, clinical presentation and potential management options was invaluable. The morning session presentations were abundant in variety and interest, including projects and audits from Cardiff University Medical Students, Welsh Paediatric trainees, and Consultants. Of highlight during this session was the fantastic prize-winning project presented by our very own WREN co-chair Dr Siwan Lloyd on head injury following infant falls on the postnatal ward – a case series. The variety in the approach to investigation and management of such patients was fascinating, especially given the high rate of CT head abnormalities of those imaged. The subsequent departmental guideline implemented at UHW will certainly help standardise care and provide more clarity and direction for management. Almost time for lunch, but of course not before the brilliant Guest Lecture from Detective Superintendent Anthony Griffiths, Head of Public Protection, Dyfed Powys Police – ‘Child Protection: The Challenges for Policy and Multi-Agency Working.’ This lecture provided an invaluable insight into the challenges often faced by the police in child protection cases. The videos and images used were extremely powerful and emphasized the great difficulties in tracking down offenders in today’s society, particularly given the huge smart phone and social media influence. After an action-packed morning of presentations and lectures it was time to refuel with a mouth-watering lunch overlooking the absolutely spectacular scenery. Coffee could be taken onto the balcony, and what a treat it was to catch up with friends and colleagues with the sound of the waves crashing onto the shore below. There was also the opportunity during this lunchbreak to visit the exhibitor stands, the main theme being cow’s milk allergy, in-keeping with the invitation lecture earlier in the day, and there were a variety of different formulas to sample at these stands (some of which far more palatable than others!!) The afternoon session was equally interesting and stimulating, including presentations inspiring and empowering trainees, highlighting the importance of blogging, social media and trainee-led initiatives to encourage learning and champion change. The final Guest Lecture of the day was provided by the highly-regarded Dr Julian Forton, Consultant in Paediatric Respiratory Medicine and Cystic Fibrosis, UHW, on ‘the new C21 Curriculum at Cardiff University School of Medicine.’ It was absolutely fascinating to learn how the curriculum and course structure has evolved since my days in medical school! The aim is for a more case-based, small group learning approach with early clinical exposure. The exam format was also an interesting change, whereby all years take the same end-of-year exam, with the focus being on demonstrating improvement and development each year. As the sun was setting at the end of a wonderful day, it was time for the evening entertainment in the form of the ‘celebrating trainee event’ followed by the formal evening dinner. This year the Best Trainee prize went to Dr Siwan Lloyd in South Wales (taking a clean sweep of prizes!) and to Dr Stacey Killick in the North. Best Educational Supervisor went to Dr Zoe Roberts…congratulations to all!
The day was wrapped up with a splendid evening of dinner and dancing (thank goodness for the spa to recover the next morning!) Once again, WPS has delivered an outstanding conference! It provides an excellent platform to showcase your work, and to become inspired by colleagues and friends. It also provides the opportunity to learn from lead professionals in their specialised field, and to celebrate the achievements of others. We certainly are lucky to have such a wonderful paediatric society in Wales! Now, who’s joining me for the Spring meeting?!.... |
Editors
Dr Annabel Greenwood Categories
All
|

























 RSS Feed
RSS Feed
