|
Dr Tom Cromarty Editor Interests: Paediatric Emergency Medicine, Medical Engagement and Leadership, Simulation, Quality Improvement, Research Twitter: @Tomcromarty |
Welsh Research and Education Network
WREN BlogHot topics in research and medical education, in Wales and beyond
Dr Celyn Kenny Editor Interests: Neonates, Neurodevelopment, Sepsis, Media and Broadcasting Twitter: @Celynkenny |
|
Katie Richards As part of my Master’s (MA) in Music Therapy and my training to become an HCPC-registered qualified Music Therapist (one of the allied health professions), I am fast approaching the end of my final placement, in a regional tertiary-level Neonatal Intensive Care Unit (NICU), which consists of an intensive care unit (ITU), a high-dependency unit (HDU), a low-dependency unit (LDU) and a nursery. Part of the requirements for our final placement, which forms most of our Advanced Professional Practice module, was that we had to set up a new music therapy service somewhere which had never had it before (one day per week for around 24 weeks). We could choose any client group or setting, and I was drawn to working with neonates ever since reading an article (scroll to see some reading recommendations!)by chance during the first year of this three-year part-time MA course. I was absolutely thrilled when the Senior Nurse emailed me back within minutes to say they’d love to have me on board! I did lots of preliminary reading around music therapy in the NICU and observed a qualified music therapist working in a different regional NICU prior to commencing my placement, so I had a pretty good idea of what to expect. As with all our placements, this involved six weeks’ observations at the start, before commencing our own clinical work. Our placements are very varied, with my first-year placement having been in a Special Educational Needs (SEN) school working with a child with autism and my second-year placement in a private psychiatric hospital working with in-patient adults with acute mental health issues (and some with complex mental health issues, e.g. chronic schizophrenia and dementia co-morbidly). This sets us up for our future work, where the client groups could be incredibly varied (from pre-birth to end of life, and everything in between). The thing about music therapy is that you usually need a wide variety of musical instruments for different circumstances. Because we often work ‘in the moment’, you just don’t know when you may need something in particular, so it’s better to have it with you than not to. Because of this, I start my day by loading myself up like a Buckaroo – one more stringed instrument and my arm might fall off! Neonatal music therapy sessions can look quite different depending on the patient you’re working with and are adjusted to what that particular baby/parent needs at that moment in time, keeping in line with their broader clinical goals. For example, when working with a term baby who was quite aware of their surroundings and in a quiet-alert state, I used musical instruments with more of a sensory impact to encourage visual tracking (e.g. the shiny, reflective tambourine, the colourful rattle or the colourful wave drum – see photo). Of course, these instruments all work on auditory stimulation, but with the added benefit of visual stimulation and tactile stimulation if the baby swipes or grabs one of these instruments. I purposely selected rattles which would be easy for tiny fingers to grip, or instruments which don’t take much physical effort to make a sound, be that with their hand, foot, arm or leg. I was careful to ensure that all of my instruments could be easily wiped clean and sterilised after working with each patient, to reduce the risk of infection. Before beginning each music therapy session, I check with the baby’s nurse (and the parent, when they’re present) if it’s okay for me to work with the baby at that time, or whether they’d rather I came back later that day or the following week. It’s important to check that it’s suitable timing, and to be able to be flexible if not. Checking what state the baby is in (whether they are fairly alert, irritable or sleeping) is also important, and determines whether or not I work with them at that moment and, if so, which instruments I would use for that session. Different instruments would be used for different states and clinical goals, and also for different aged babies.
For babies born at very early gestational ages (e.g. 25 weeks), if they’re not many weeks old yet I tend not to work with them. Their mother’s voice will be the best and safest thing for them to listen to, whether that is through talking, humming or singing quietly. It’s crucial not to over-stimulate very young babies, as they need to adjust to the world first, which takes time. The sensory input from bright lights, noises around the ward, smells and touch can be too over-stimulating if they all occur simultaneously. It can calm them just hearing Mum’s voice (and indeed her heartbeat), whilst feeling the vibrations of her voice and heartbeat during skin-to-skin time. With this aged baby, I would only offer emotional support to the parents, and provide suggestions of how they could use humming/gentle lullaby singing, or even just reading or talking to their baby to support their wellbeing and development at that time, being sure to let parents know to watch out for signs of over-stimulation in their baby, explaining what these might be. For babies born at gestational ages such as 34 weeks, I might work with them while their parent is holding them. In this scenario, I would use gentle (and very simple) guitar playing with just two chords, often accompanying improvised quiet singing (e.g. singing “Jacob, Jacob, how are you today?” [don’t worry – no actual patients’ names have been used in this example!]). I try to encourage parents to sing or hum along quietly, but often find that they are perhaps too embarrassed or self-conscious to do so on the ward, which I can completely understand. It’s not the same as being at home and having your own space, with no-one else watching or listening to your every move while you try to get to know your baby. Research has shown the importance of using the mother’s own voice, as this is what the baby will respond to best. The familiar sounds from being in utero (the whooshing of the amniotic fluid, the strong pulse of the mother’s heartbeat and the muffled sounds of the mother’s own voice, as well as those of people she sees regularly – so often the father’s voice is also recognisable to the baby) create a feeling of security for the baby as it tries to adjust to its new surroundings, so re-creating this in an informed and cautious way whilst watching for any signs of over-stimulation is important. During the music therapy session, I’m constantly looking out for any signs of over-stimulation (there are many!) and checking the baby’s monitor for their heart rate, oxygen saturation levels and respiratory rate, which further helps me to assess their mood and current state. I also check the sound levels of my musical interaction via a decibel-monitoring device. With a more relaxed baby comes development, the ability to sleep and feed better and better emotional wellbeing, which is crucial for the often-traumatic environment they now find themselves in. The gato box (see photo – the two-tone wood block) is used to gently re-create sounds of the mother’s heartbeat, and with this you can help the baby to entrain their own heartbeat to a slower pulse, inducing relaxation and often sleep. Using the wave drum (see photo – the oceanic disc, complete with cartoon octopus!) very slowly and quietly (this can take a bit of mastering in itself!) can re-create sounds of the amniotic fluid whooshing around, also helping to calm the baby, reminding them of a time where they felt safe, secure and contained. The music has the power to ‘hold’ them when they are not being physically held, which is also a really effective way of helping them to feel safer. The predictable characteristics of the music, when used in an informed and careful clinical way by a trained music therapist, are purposefully used to help the baby feel more relaxed. When there is a predictableconstant for a period of time (the non-alerting style of the music used), the baby is less likely to become startled by the unpredictablesounds of bins closing, taps running, monitors beeping, doors closing and telephones ringing etc., as they have that predictable sound (the music) to tune into, which provides a sense of security. It’s also important for my sessions to be quite short – often 10 minutes is plenty. I observe for any signs of over-stimulation and bring the session to a close sooner if this occurs. For term babies who are quite alert and aware of their surroundings, perhaps having been on the unit for a while and becoming increasingly bored by the blank white ceiling tiles above them, I work with them in order to increase neuro-development, where sensory stimulation is key. I would most likely use the reflective tambourine (see photo), the easy-grip rattle (see photo) and the wave drum, as well as my guitar and voice. Simple nursery rhymes with lots of repetition can help with early language development. The rattle, wave drum and tambourine are good for visual tracking, and any of these can be used to encourage them to move their arms and legs more, building up their physical development as they reach out to touch them. Music and sounds used can also encourage a baby who usually only looks to one side to explore the other side too, which can be good for their physical development. When the baby touches one of the instruments, it can also teach them about cause and effect, as they learn that when they touch it, it makes that sound. It can also help babies to learn the (unwritten) ‘rules’ of conversation – they make a sound, then I make a sound, then it’s their turn again, then mine, and so on. This can also provide them with a sense of security – the anticipation of knowing whether they will get their turn again, consistently having those needs successfully met, builds trust and a secure attachment, which is important for their future development, and can last long into adulthood. It can be a bit of a balancing act at times, as I have sometimes worked with term babies who have been on the unit for quite some time who need sensory stimulation and a more lively session, yet they’ve been on the same ward as a baby who is only 28 weeks (gestational age) (e.g. in ITU). In this case, I factor in the rest of the babies on that ward, whilst trying to tailor the sessions to the individual baby I’m working with, so ensuring I’m quiet and perhaps sticking more to guitar and singing simple nursery rhymes, or improvised observational singing based on what the baby is doing, whilst slowly moving the rattle from left to right for the baby to track it visually. I often leave them a small square cut from some thin emergency blanket material (bought especially for this purpose) to play with (supervised!) on the days I’m not there – it makes a fascinating crinkly sound and is very cheap, as toys come! After each session I sanitise the musical instruments, then have to negotiate the notes… who knew it could be such a mammoth task adding a new continuation sheet half-way through a patient’s file?! I attend the MDT meeting when possible, where most of the patients are discussed. This helps me to be more informed about the family situation of the babies (including any psycho-social issues), and also helps me to prioritise who to work with (babies andparents). A big part of my clinical work on the NICU, which people may not initially think of, is talking to (and, more importantly, listeningto) parents and providing much-needed emotional support to them. I also ran a music therapy support group for parents, using relaxation techniques and providing a confidential space for them to meet other parents and explore their experiences on the NICU, using music to help in the process. Parents can be experiencing trauma in the NICU, so it’s vital to provide that emotional support, which can be invaluable for helping them cope. Some parents don’t necessarily have much of a support network around them in the form of friends and family, so it’s important for them to have someone to talk to. We have regular confidential clinical supervision and peer supervision, as well as clinical seminars in university. This helps us to think about the work in different ways, which ensures it remains patient-focussed and helps to achieve clinical goals. Reflective practice also plays a big part in our work as music therapists. If you’d like to get more of an idea of how music therapy sessions look in NICU work, you can watch these two short videos on YouTube (though they’re from America, so it’s not exactly the same): https://youtu.be/bwKCK3W-96E https://youtu.be/4qjx2BrrQJg Reading recommendations: Loewy, J., Stewart, K., Dassler, A., Telsey, A. and Homel, P. (2013) The effects of music therapy on vital signs, feeding, and sleep in premature infants. Pediatrics. 131 (5), pp. 902-918. Loewy, J. (2011) Music therapy for hospitalized infants and their parents. In: Edwards, J., ed. (2011) Music Therapy and Parent-Infant Bonding. Oxford: Oxford University Press, pp. 179-190. Shoemark, H., Hanson-Abromeit, D. and Stewart, L., (2015) Constructing optimal experience for the hospitalized newborn through neuro-based music therapy. Frontiers in Human Neuroscience. 9: 487.
2 Comments
Dr Tom Cromarty The term “Burnout” has become somewhat of a dirty word in the healthcare lexicon over the last few years. The insinuation that healthcare staff have somehow failed to build enough resilience or resourcefulness to manage the stressors of life on the front-line. The concept of “front-line” comes from war battlefields and it’s no co-incidence that this metaphor is used in healthcare. Soldiers get diagnosed with PTSD, whilst healthcare professionals suffer burnout. Both of these have at their core the issue of “Moral injury”. If doctors were “in it for the money” then I’m pretty sure they would be astute enough to pursue another line of work. Caring for patients and their families is a vocation for most doctors, or at least it started off that way at some point in the “life choices” decision making process. However, when doctors are not able to deliver the high standards of care they intended for a variety of reasons, this takes a toll on personal wellbeing. The symptoms of burnout are really a “signal” of a healthcare system that is failing to look after its assets. If we want compassionate, engaged and highly skilled doctors leading the charge on the frontline then we need to provide the working environment to facilitate it. This starts with senior leadership recognising that >50% of doctors are experiencing these symptoms and they “Cannot give what they don’t have”! Many organisations now recognise the urgency of the situation and are starting to offer support. However, there are a number of skills which we can develop as individuals to equip us for “combat in the healthcare battlefield”. I have looked up to Dr Mark Stacey for a number of years. An obstetric anaesthetist and human factors expert, he has put together a “Bakers Dozen” of skills. Written as a prescription to yourself, these can all be practiced and developed, in our quest for becoming “Anti-Fragile” (the opposite of fragile funnily enough). I have been lucky enough to hear this talk a couple of times, taking new learning points from it on each occasion. I would highly recommend contacting [email protected]and see the talk in person, but in the meantime here is a short summary of 'The Baker’s Dozen' by the legend himself; 1. Problems: challenge or threat? Do you view your problems as a challenge or a threat? From a practical (and physiological) point of view it is more useful to frame problems as a challenge (problem solving mode) versus a threat (fight/flight mode). This also means reflecting on your self-talk about life eg “life is unfair”, sadly we know that, we see proof of it on a daily basis. 2. Develop optimism skills even if you are a pessimist Having started out researching ‘learned helplessness’ (something many in the NHS will be familiar with, especially our patients), Marty Seligman has become a top optimism guru. His PERMA model (Positive Emotion, Engagement, Relationships, Meaning, Achievement) is helpful. I have also found the ‘Losada principle’ very useful - three nice things to balance/overcome one negative (unless of course if you’re in a long term relationship....). The PERMA Model: Your Scientific Theory of HappinessAlso, have your own mission statement and rehearse it daily. Mine is “today I am going to do the best I can for my family and the people I care for”. 3. Keep a gratitude diary What 3 things have you done well in the last 24 hours? I usually think about these on the way home from work, which sets me up to start the evening in a positive manner. How many of you when you get home complain to your partner? Flip it round – say or do something positive. 4. Do physical exercise (every day) Do not underestimate the benefits of regular physical exercise. Lack of time is an often used excuse, but do you have time not to exercise when you look at the range of benefits (decreasing risk of Alzheimer’s, improving mood, improved sleep and many others)? The 7 minutes exercise app is a great way of moving all your body parts without taking up too much of your time. 5. MEDITATE Probably the most useful skill I have learnt in the last 25 years – it has a whole range of benefits; improved concentration, focus and sleep. If you don’t do some form of meditation you are spending less time on your mental health than you are cleaning your teeth! The simplest meditation technique I have found is the four count breath technique also called box breathing. It only takes a minute – breathe in for a count of 4, hold for 4, out for 4, hold for 4 – do 4 times – perform when you feel that acute pressure coming on and practice every day – teach it to everybody! (Even the Navy Seals are taught it!) 6. Become a stress management expert Imagine a bucket, while at work fill it with the stressors of the day, at the end of your shift find a trigger (for me it is unlocking my bike) to empty the bucket. Now you are going home with an empty bucket ready to be filled with the stressors of home. Set a second ‘empty bucket’ trigger (like brushing your teeth before bed) to set you up for the next day and of course... “Scientists have discovered a revolutionary new treatment that makes you live longer. It enhances your memory, makes you more attractive. It keeps you slim and lowers food cravings. It protects you from cancer and dementia. It wards off colds and flu. It lowers your risk of heart attacks and stroke, not to mention diabetes. You’ll even feel happier, less depressed and less anxious. Are you interested?” (see number 7) 7. Sleep! The above quote is from Matthew Walker’s recent book and if that hasn’t convinced you then I’m not sure that I will. Sleep – ignore it at your peril, it is possibly the most important performance enhancing agent available to you. 8. Ask for Help Never be afraid to do this whether you are a senior consultant or newly appointed trainee. 9. Deal with aggression Learning assertive skills is worth the effort particularly as there will always be conflict in our jobs. 10. Learn Learning is a fantastic skill that does not just teach us the skill – it also teaches us about learning – in particular how, as an expert, it is difficult to understand why the novice is struggling to learn the skill. 11. Make better decisions You could read the enjoyable and academic “Thinking Fast and Slow” by Daniel Kahneman or more readable “Decisive” by Chip and Dan Heath that teaches the WRAP model. In particular note the prepare for failure – we can do everything right in our job but bad things will still happen. 12. Avoid HALT in you and the people you work with Are you Hungry, Angry, Late or Tired? Avoid these factors in yourself and look out for them in your co-workers/friends/partners/ children. They will look out for HALT in you. The HALTcampaign, lead by Michael Farquhar and Guy’s hospital, is a model worth following. 13. Smile As you work through your day see how many people you can make smile. …..And there you have it.
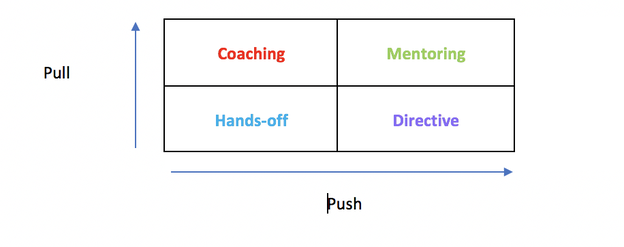
These are all skills! And as such they will all get better after practice and less easy when neglected. Just get started and have a go at two or three of them. I have found the gratitude diary and sleep (earlier bed times) particularly useful in recent weeks and have seen benefits in my overall wellbeing. Mark reminded us that if you never meditate, you are spending more time cleaning your teeth than on your mental health. Some people say “We don’t have time for any of this” but the truth is “We don’t have time to neglect it”. If you want to be the compassionate, healthy, high performing doctor you always dreamt of, the remember “You can’t give what you don’t have!” Baker’s Dozen of Mental Toughness. Your stress management and resilience toolkit The Happy MD – Dr Dike Drummond Mission Statement: Revolutionize the quality of healthcare by improving the health, happiness, humanity and effectiveness of the people providing patient care. Physician Burnout Symptoms ZDoggMD – Moral Injury Reading List from Mark Stacey: Human factors and resilience Mastering Resilience in Oncology: Learn to Thrive in the Face of Burnout. Fay J. Hlubocky, PhD, MA. Miko Rose, MD, and Ronald M. Epstein, MD Practical Human Factor training Martin and Elaine Bromiley – “How mistakes can save lives” Decision making and brain training! Brain rules: John Medina The Decisive moment: Jonah Lehrer Decisive: Chip and Dan Heath Three books: three slightly different takes on human error Safety at the Sharp end: Rhona Flin Field guide to understanding Human error:Sydney Dekker Why hospitals should fly-much lighter than the above: Nance J. Mind management recommendations: The Chimp Paradox: Steve Peters (it works for the Sky cycling team) Search inside yourself: Chade Meng Tan (it works for google!) 10 % happier - Dan Harris- true life story with loads of practical advice-advice-done be put off by the title! 26th March 2019, Cardiff Dr Annabel Greenwood ST4 I am currently in the process of implementing a mentorship programme on the Neonatal Unit at UHW. As a trainee, it’s hard not to feel overwhelmed and at times, emotionally drained by the demands and expectations of our training. Our wellbeing and a positive mindset are paramount in ensuring we can optimise our potential, but how can this be achieved without an appropriate support network in place? Last month, I was fortunate enough to attend the RCPCH Mentoring Skills Workshop in Cardiff to learn more about mentorship and the key principles involved. This was a fantastic one-day workshop lead by Matt Driver and Sandra Grealy, who have a wealth of experience in coaching and leadership. I feel passionately that mentorship is an invaluable process for both the mentor and the mentee, and would like to use this platform to share with you some of the key concepts involved… So what is mentoring? Mentoring is the process of supporting and guiding a mentee in the development of their own ideas and agenda. The mentor is usually a more experienced professional who aims to help nurture the potential of the mentee. The Situational Model The relationship between a mentor and mentee relies on the right balance between ‘push’ and ‘pull.’
This balance helps us understand the differences between coaching, mentoring, directing, and a more hands-off approach. Depending on the situation and the needs of the person, the balance between ‘push’ and ‘pull’ will need to be adjusted accordingly; Coaching: The agenda is set by the coach rather than the subject. ‘Pull’ behaviours outweigh ‘push’ in this case. Directive: The agenda is set by the ‘director.’ It is an important approach where the subject needs to have information. ‘Push’ behaviour outweighs ‘pull.’ Hands-off: The subject is encouraged to do things for themselves, without ‘push’ or ‘pull.’ Core SkillsSo, what are the key core skills to be an effective mentor?
What about advice? Let’s face it, if someone comes to you with a problem, it’s all too easy to jump-in with our own opinion or advice, often backed up by personal experiences. However, this approach is not useful in the case of mentoring, as it discourages the mentee from exploring their own possible options or solutions and driving their own agenda. During the workshop we worked through a useful exercise to help appreciate this difference.
After listening to the mentee, the mentor was given the task of adopting two different approaches; a) Give advice b) Work through a structured set of questions instead;
As you can see, approach b) focusses on ‘success’ and positivity. These are open questions, allowing the mentee to create and explore their own agenda. The ‘T-GROW’ approach to mentoring The ‘T-GROW’ pneumonic provides a very useful structure to shape a mentoring session; Topic
Goal
Reality
Options
Will
The Contract Before embarking on a mentorship session it is important to address ‘the contract.’ This defines the relationship between the mentor and the mentee, and provides the opportunity to explore each other’s expectations at the outset. It is important to emphasise the confidential nature of the meeting, unless of course any alarming information is shared. How do I learn more?
|
Editors
Dr Annabel Greenwood Categories
All
|







 RSS Feed
RSS Feed
