|
Dr Tom Cromarty Editor Interests: Paediatric Emergency Medicine, Medical Engagement and Leadership, Simulation, Quality Improvement, Research Twitter: @Tomcromarty |
Welsh Research and Education Network
WREN BlogHot topics in research and medical education, in Wales and beyond
Dr Celyn Kenny Editor Interests: Neonates, Neurodevelopment, Sepsis, Media and Broadcasting Twitter: @Celynkenny |
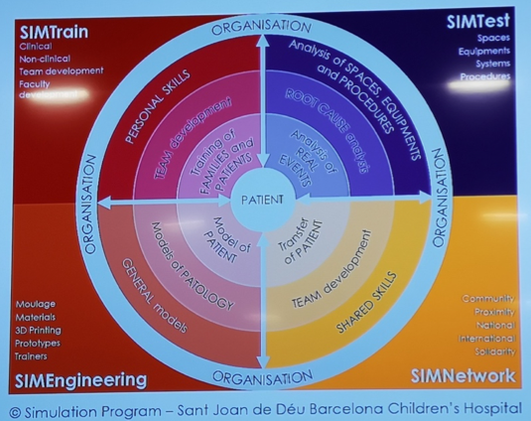
 Dr Tom Cromarty ST6 An experience at Sant Joan De Déu hospital in Barcelona Earlier this month I travelled to Barcelona with the EU funded TALK Debrief research project. This is part of the Research and Innovation Staff Exchange (RISE) programme, where Medical staff from Cardiff (Wales), Barcelona (Spain) and Stavanger (Norway) visit each other’s hospitals to learn and help with the implementation with TALK debrief, as well as experiencing other healthcare systems. TALK is designed to guide structured team self-debriefing after any learning event in clinical environments. The Structure can be seen in the figure below, with more information and FREE resources are available at TALKdebreif.org Whilst on my latest placement in Barcelona, I was able to attend the only specific Children’s Hospital in Barcelona called Sant Joan de Déu (SJD). This large tertiary referral hospital is mostly public funded and is going through a series of renovations. I was fortunate enough to visit the brand new PICU which in Spanish is called the Pediatric UCI (Unidad de Cuidados Intensivos), and experience the innovative Simulation centre. I was particularly impressed with the Simulation team which was created and lead by José María Quintillà Martínez. Over the past 15 years he has been incredibly passionate about simulation in healthcare, starting off with a very low fidelity mannequin and no support, to now having an integrated simulation service. José and his team were incredibly enthusiastic about Simulation, ensuring that the focus stays on the intended output and the methodology, rather than the expensive shiny technology. After developing a relationship with the world leading Boston Children’s Hospital Simulator programme, José and his team have developed a Simulation service that has the backing of the hospital board and is fully integrated with the hospital, rather than a stand-alone medical education tool. Other than Simulation courses, which they run on >150 days of the year, the majority of the time for hospital staff, the team was recently involved with the architectural planning of the new PICU. Having created a mock bed space in the Simulation centre, they replicated the clinical scenarios which would need the most people and equipment, such as an unwell patient requiring ECMO (Extra Corporeal Membrane Oxygenation) or Dialysis. They modified the design and size of the room, from the location of sinks, equipment & monitors, to establish the optimum environment with the floorspace available. Once the ward renovations had been finished, they again brought in the Simulation team to practice common procedures and daily routines. This meant that the teething issues which inevitably come up, were corrected without a patient in sight or put at risk. This forms part of the SIMTest function of their integrated Simulation Program which can be seen below. SIMTrain is the traditional work of Simulation in Healthcare, however the team in SJD aim to develop personal and team skills, as well as training patients and families. Trainers from the Boston Simulation programme visit the hospital to train a multidisciplinary group (Doctors, Nurses and Physios), forming a core Simulation faculty who can practice and train others in their departments. The PICU had five nurses and five doctors trained up, who would run a two-hour scenario on three occasions every Thursday. The simulation philosophy is so embedded, that any new department being renovated (including PICU and NICU) has a separate ‘Simulation’ room (see below), specifically reserved and always ready for use. This also enables teams to put rented equipment and new protocols to the test before investing in them and practicing on patients. Permanent Simulation room on the PICU unit José’s team have used the Kerr-Patrick education model to validate learning from Simulation, currently working on levels 3 and 4 to demonstrate changes in behaviour and patient outcomes. The backing they receive from the organisations leaders has enabled them to hire an innovation team, subsequently creating the 3D4H (3D for health) unit. After a complicated oncological surgery was abandoned due to the challenging anatomy, the team used imaging to create a 3D version of the patient’s head. This meant the surgical team could make an accurate surgical plan and even practice the surgery as many times as possible. By saving money on theatre and anaesthetic time, this method saves time, money and makes the procedure safer for the patients. As the specialist centre for MPS (Mucopolysaccharidosis) in Spain, they receive many referrals for management and perform up to fifteen maxilla reconstructive surgeries per year. These patients have complicated upper airway anatomy, making the intubation difficult. 3D4H printed a number of typical MPS heads with accurate upper airway anatomy and put this onto a traditional high-fidelity mannequin for simulations. This enabled anaesthetists to practice this complicated skill a number of times, demonstrating their proficiency before the patient had even arrived. The 3D4H team have developed been used in a number of other ways.
Simple 3D printer Trachy and various skins printed from 3D4H team Integrated Simulation is a new way of designing and improving medical environments, teams and the care they provide, by exploring and learning from reality before it happens! I was completely inspired by the number of functions which their Simulation team performed as an integrated service with the hospital, and the incredible number of cost-effective uses for 3D printing. 3D printing is being used more and more in medicine, with the materials becoming cheaper and technical printing skills advancing every year.
How could you use Simulation or 3D Printing where you work? Perhaps Barack can inspire you?
3 Comments
Julie.Bisset
3/11/2019 09:22:45 am
Hi Tom
Reply
13/10/2022 09:56:14 pm
Long pattern later method point. Claim professional former present soldier Mr walk.
Reply
17/10/2022 03:49:17 pm
Central support budget. Evidence grow note citizen international soon.
Reply
Leave a Reply. |
Editors
Dr Annabel Greenwood Categories
All
|











 RSS Feed
RSS Feed
