|
Dr Tom Cromarty Editor Interests: Paediatric Emergency Medicine, Medical Engagement and Leadership, Simulation, Quality Improvement, Research Twitter: @Tomcromarty |
Welsh Research and Education Network
WREN BlogHot topics in research and medical education, in Wales and beyond
Dr Celyn Kenny Editor Interests: Neonates, Neurodevelopment, Sepsis, Media and Broadcasting Twitter: @Celynkenny |
|
Key themes from this year’s annual conference were investing in the workforce and the future paediatrician with many plenaries and breakout sessions having a focus on staff wellbeing. Considering the ever increasing number of articles regarding dissatisfaction and junior doctor burnout, and the well-known case of Dr Bawa-Garba it was a pleasure to see the college taking on board the struggles of trainee wellbeing and taking the occasion to explore this further. It was an enjoyable experience to have the opportunity to listen to so many inspirational speakers and hear their experiences and to discuss the projects that they had been involved with. For the early risers, Tuesday morning began with a 5K run or a yoga session – I have to admit that I wasn’t there for either due to being on a train but I thought a nice session to include in the programme and begin the day with, and so I hear enjoyable. "Learning from Excellence"Dr Adrian Plunkett, Consultant Paediatric Intensivist in Birmingham, gave the initial plenary session on “Learning from Excellence” for what proved to be a highly motivational talk. He discussed how for so long the focus of health care has been avoiding harm and improving care, by learning from errors already made. He feels it is almost ingrained within us as part of our training to find the mistake, rather than focussing on the positive. He gave the example of a series of sums, and asked the audience what we saw: Honestly, what did you focus on first? The one wrong calculation, or the four that were correct? His take was that we should be taking the time to appreciate and reward excellence and hard work as a way to learn, rather than focussing on what an individual or organisation has done wrong. “Success has a much greater influence on the brain than failure” - Earl Miller (MIT Neuroscientist) Dr Plunkett wants us to ask ourselves, when regarding our peers and colleagues:
His group were the first to spearhead the emerging certificates of appreciation and now has a whole group focussed studying excellence in healthcare to help create new opportunities for learning and improving resilience and staff morale. For those interested www.learningfromexcellence.com and I believe a conference in the planning for February 2020. "The Cost of Caring"Dr Hilary Cass (previous RCPCH president) and Dr Caroline Elton (psychologist and author of “Also Human”) lead a stimulating seminar exploring how the traditional view of patient-centred care wasn’t enough, and more consideration needed to be given to the health professionals providing that care. The “Triple Aim” was an initiative designed to optimise health performance by focusing on (unsurprisingly) three aims - enhancing patient experience, improving population health, and reducing costs. BUT... It is increasingly felt that this is not enough and many organisations are now moving towards the “Quadruple Aim” with the fourth aim being the goal of improving the work life of health care providers. Dr Cass spoke about doctors, and particularly paediatricians being over-represented in those that access professional counselling services. Anecdotally, she describes paediatricians being at higher risk of stress, burnout and depression than some specialities but at lower risk of addiction to alcohol or drugs. Dr Elton discussed her book which many members of the audience had read and appreciated and then discussed her own practice, particularly focusing on career planning for doctors and helping doctors make the right decisions for them when trying to balance the work and lives. www.careerplanningfordoctorsanddentists.com "How does burnout affect patient care?"Dr Judith Johnson (psychologist) discussed causes of burnout and expressed what the majority of healthcare workers are feeling. Many causes of burnout were identified and discussed – excessive workload, low staffing levels, poor leadership, lack of support and lack of resources. These are known, accepted and still people have difficulty challenging that this isn’t right or appropriate. She gave the example of the Mid-Staffordshire inquiry “when staff are burnt-out terrible things can happen”. Burnt out and disengaged staff were present on all levels resulting in a catalogue of events and lack of care. "Wellbeing"Dr Dan Magnus (PED Consultant, Bristol) kicked off the trainees’ session with a lively discussion on wellbeing within medicine. Opening with a comparison between doctors and the crew of Apollo 13. I’ll admit I was slightly alarmed by this statement as I didn’t think things were that bad, only to realise later I’d mixed up Apollo 13 with the Challenger spacecraft disaster, and rather than our careers coming down in flames it was more – “Medicine you got a problem”.
Dr Magnus has done much work, particularly in ED, looking at the need for recovery after shifts and traumatic scenarios. Taking 10 minutes and having a cup of tea after a difficult event is not enough. He described working in Toronto where doctors don’t work more than 2 long day shifts or nights in a row (living the dream)! www.yougotthiswellness.com/ He describes three essential components of wellbeing within the NHS – belonging, competence and autonomy. Perhaps surprisingly he’s not particularly a fan of resilience training “encouraging doctors and medical staff to ‘be more resilient’ is just a crafty way of diverting attention from understaffed rotas and deteriorating working conditions in an effort to get individuals to be more accepting of clinical environments”. He highlights one of the main barriers to improving wellbeing as establishing what people want as every doctor or health professional will have a different take on what’s important to them. Saying that the general view is: better rotas, better facilities for rest and relaxation and more civility and kindness in the workplace”. He identified 5 key statements for improving wellbeing:
www.emtraineesassociation.co.uk/fatigue-shift-work--rotas http://www.emtraineesassociation.co.uk/rest Overall, an enjoyable conference with lots of food for thought!
0 Comments
Leave a Reply. |
Editors
Dr Annabel Greenwood Categories
All
|







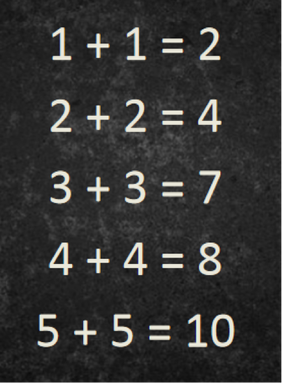
 RSS Feed
RSS Feed
